
Percutaneous aortic valve replacement (PAVR), also known as transcatheter aortic valve implantation (TAVI) or transcatheter aortic valve replacement (TAVR), is the replacement of the aortic valve of the heart through the blood vessels (as opposed to valve replacement by open heart surgery). The replacement valve is delivered via one of several access methods: transfemoral (in the upper leg), transapical (through the wall of the heart), subclavian (beneath the collar bone), direct aortic (through a minimally invasive surgical incision into the aorta), and transcaval (from a temporary hole in the aorta near the belly button through a vein in the upper leg).
Severe symptomatic aortic stenosis carries a poor prognosis. Until recently, surgical aortic valve replacement was the standard of care in adults with severe symptomatic aortic stenosis. However, the risks associated with surgical aortic valve replacement are increased in elderly patients and those with concomitant severe systolic heart failure or coronary artery disease, as well as in people with comorbidities such as cerebrovascular and peripheral arterial disease, chronic kidney disease, and chronic respiratory dysfunction.

Maps, Directions, and Place Reviews
Medical uses
A systematic review of low and intermediate risk people showed that transfemoral TAVR probably reduces short-term risk of death, stroke, life-threatening bleeding, but increases the risk of heart failure symptoms and slightly increases the need for a reintervention. The same review found credible evidence that transapical TAVR probably increases the risk of death, stroke, acute kidney injury, pacemaker insertion, and slightly increased need for reintervention compared to surgical aortic valve replacement. Longterm TAVR valve durability >5 years remains unknown, especially relevant to patients with a longer life expectancy.
Transapical TAVR should only be used in extreme circumstances: an evidence-based BMJ Rapid Recommendation made a strong recommendation against transapical TAVR in people who are also candidates for either transfemoral TAVR or surgery. People who have the option of either transfemoral TAVR or surgical replacement are likely to choose surgery if they are younger than 75 and transfemoral TAVR if they are older than 75. The rationale for age-based recommendations is that surgical aortic valve replacements are known to be durable long-term (average of durability of 20 years) so people with longer life expectancy would be at higher risk if TAVR durability is worse than surgery.
Transcatheter Heart Valve Video
History
The catheter procedure was developed in France, initially performed in 2002 on April 16 by Prof Alain Cribier in Hopital Charles Nicolle, at the University of Rouen. It is now approved in more than 50 countries. It is effective in improving functioning in the patients with severe aortic stenosis. In the US, it received FDA approval in November 2011 for use in inoperable patients and in October 2012 for use in patients at high surgical risk.

Devices
Medtronic's CoreValve Transcatheter Aortic Valve is constructed of a self-expanding Nitinol frame and delivered through the femoral artery. This device received FDA approval in January 2014.
Boston Scientific's Lotus Valve system was awarded CE approval in October 2013. It allows the final position to be assessed and evaluated before release and has been designed to minimise regurgitation.
St Jude Medical's Portico Transcatheter aortic valve received European CE mark approval in December 2013. The valve is repositionable before release to ensure accurate placement helping to improve patient outcomes.
Edwards' Sapien aortic valve is made from bovine pericardial tissue and is implanted via a catheter-based delivery system. It is approved by the FDA for use in the US.

Implantation
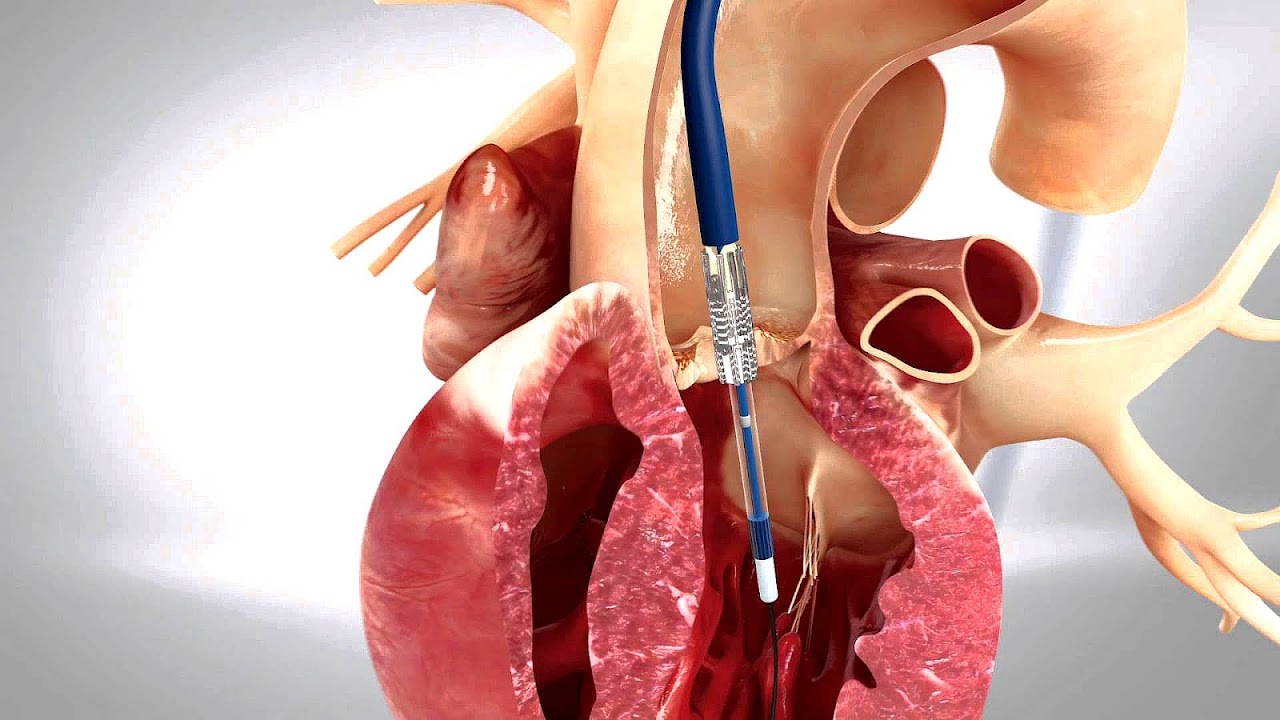
The devices are implanted without open heart surgery. The valve delivery system is inserted in the body, the valve is positioned and then implanted inside the diseased aortic valve, and then the delivery system is removed. The catheter based delivery system can be inserted into the body from one of several sites.
The transfemoral approach requires the catheter and valve to be inserted via the femoral artery. Similar to coronary artery stenting procedures, this is accessed via a small incision in the groin, through which the delivery system is slowly fed along the artery to the correct position at the aortic valve.
The transapical approach sees the catheter and valve inserted through the tip of the heart and into the left ventricle. Under general anesthesia, a small surgical incision is made between the ribs, followed by a small puncture of the heart. The delivery system is then fed slowly to the correct position at the aortic valve. The puncture in the heart is then sutured shut.
The transaortic approach sees the catheter and valve inserted through the top of the right chest. Under general anesthesia, a small surgical incision is made alongside the right upper breastbone, followed by a small puncture of the aorta. The delivery system is then fed slowly to the correct position at the aortic valve. The hole in the aorta is then sutured shut.
The transcaval approach has been applied to a smaller number of patients who are not eligible for transfemoral, transapical, or transaortic approaches. In the transcaval approach a tube is inserted via the femoral vein instead of the femoral artery, and a small wire is used to cross from the inferior vena cava into the adjacent abdominal aorta. Once the wire is across, a large tube is used to place the transcatheter heart valve through the femoral vein and inferior vena cava into the aorta and from there the heart. This otherwise resembles the transfemoral approach. Afterwards, the hole in the aorta is closed with a self-collapsing nitinol device designed to close holes in the heart.
Source of the article : Wikipedia

EmoticonEmoticon